Tregoning
12 April 2024 | We are back aboard Tregoning in Mersin Marina, Mersin, Türkiye
02 April 2024 | We are in Toronto Airport, Canada: Tregoning is in Mersin Marina, Mersin, Türkiye
25 February 2024 | We are back in Gainesville, FL: Tregoning is in Mersin Marina, Mersin, Türkiye
18 February 2024 | We are in Glenwood, New Mexico: Tregoning is in Mersin Marina, Mersin, Türkiye
12 February 2024 | We are in Morro Bay, California: Tregoning is in Mersin Marina, Mersin, Türkiye
19 January 2024 | We are in Vancouver, BC Canada: Tregoning is in Mersin Marina, Mersin, Türkiye
01 January 2024 | We are in Washington State: Tregoning is in Mersin Marina, Mersin, Türkiye
15 December 2023 | We are in Minnesota: Tregoning is in Mersin Marina, Mersin, Türkiye
18 November 2023 | We are in Florida: Tregoning is in Mersin Marina, Mersin, Türkiye
29 October 2023 | We're in Florida - Tregoning is at B-dock, Mersin Marina, Mersin, Türkiye
21 October 2023 | 7 Oda Kapadokya Cave Hotel, Ürgüp, Türkiye
14 October 2023 | Hotel Aşikoğlu, Boğazkale, Türkiye
07 October 2023 | B-dock, Mersin Marina, Mersin, Türkiye
19 September 2023 | “Chez Jon & Angela”, Near Otterton, Devon, UK
14 September 2023 | Airbnb in Fortuneswell on the Isle of Portland, Dorset, UK
11 September 2023 | With Mike, Grange-over-Sands, Cumbria, UK
03 September 2023 | Ardington House, Ardington, Oxfordshire, UK
24 August 2023 | Near "Chez Joan and Peter", College of Roseisle, Moray, Scotland
11 August 2023 | Andrew's house (not exactly), Lichfield, UK
22 July 2023 | Chez Gail, near the New York Café, Budapest, Hungary
A significant change in plans
26 January 2016 | Tregoning is in Whangarei Town Basin Marina, Whangarei, New Zealand but we are in Gainesville, FL
Photo: Randall with his heart pillow just before his by-pass surgery
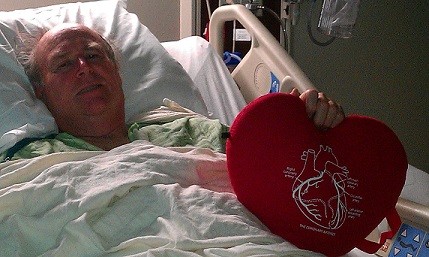
During a couple of bike rides in Whangarei, Randall had found himself with a racing heart and gasping for air when we exerted ourselves on an uphill stretch. While it was tempting (for me) to assign this to a shortfall of rigorous exercise over the holidays, he told his doctor that he would like a stress-test as part of his annual physical. So on Tuesday (January 19th), after a routine visit to his GP, Randall was booked to see a cardiologist for an EKG. While this showed that his heart seemed to be fine when at rest, a stress-test was arranged for the next morning. This test indicated that his heart muscles were in good shape but there did seem to be some issues with the shortness of breath while on the treadmill and with his near-fainting while in the waiting-room after the rigorous exercise.
So Thursday morning found us in a prep-room at the North Florida Regional Medical Center with Randall being readied for a heart-catheterization to inspect the state of the arteries providing blood to his heart. This was accomplished by a catheter inserted through his wrist and if there was any indication of arterial narrowing, a stent could be inserted immediately to open-up the vessel.
While Randall was wheeled upstairs for this procedure, I scurried across the street to have a routine mammogram (all good). On my return, I was a bit surprised to find Randall back in the prep-room receiving a chest x-ray and the staff looking rather less cheerful than when I had left. Imagine my surprise when the doctor showed me the images on his cell-phone that displayed two constrictions in Randall's left anterior descending artery, a vessel that feeds the left side of the heart, one of these being a 99% blockage. This artery supplies blood to such a large volume of heart-muscle that an obstruction in it is, rather disconcertingly, called a widowmaker because a complete blockage can result in a massive heart-attack and sudden death.
Of course, if I was surprised, Randall must have been completely shocked by the sudden flurry of tests that were being applied to him. He was not going to be allowed to leave the hospital but within a few hours he was wheeled upstairs to a room in the Cardiac-Vascular Unit which was going to be his home for the next few days. Open-heart, triple by-pass surgery was scheduled for the next morning so he had to undergo his third morning in a row of fasting.
Wow...what an unexpected change of plans this was turning out to be.
Randall's operation started just after noon on Friday and lasted for four hours. While I was in the Cardiac waiting-room, I was joined by my good friend Marilyn, who had been visiting her mother-in-law, Joan, who was recovering from double-pneumonia on the floor below. The surgeon reported that Randall's procedure had gone well very well and I was allowed to see him soon after he was returned to his room, while he was still on the ventilator and surrounded by pumps and monitors. Later in the evening, I saw Randall again when he was already off the ventilator and was able to recognize me and mouth “Hello” despite the heavy dose of pain-killers. I was able to return to Karen's knowing that Randall was in excellent hands and doing well.
Early on Saturday, I found that Randall was already sitting in a chair, which is an important part of the progression after heart-surgery, along with the regular use of inhalation- and exhalation-therapy devices (one of which sounds like a rather congested duck). He was pretty sleepy all day so I was able to catch-up with various friends between visits.
Arriving early on Sunday, I was a bit surprised to find him using an oxygen mask. Apparently, he had felt a bit dizzy when he been encouraged to walk at 4:30 am. Walking is a critical part of the post-heart-surgery therapy so it is attempted several times each day and is carefully monitored. When it was time for his walk at noon, I accompanied him and his nurse down the hallway and he seemed to be doing really well but as we started returning to his room, he declared that he had gone too far and started to crumple. Sally and I caught him and lowered him to the floor so that he did not hurt himself but I was pretty frightened when one of the many nurses that suddenly appeared from the neighboring Critical-Care Unit asked whether he had suffered a stroke.
Thankfully Randall quickly regained consciousness and was immediately able to squeeze his hands and move his feet as directed. His pulse and blood-pressure were at acceptable levels but for some reason, the concentrations of oxygen in his tissues had dropped too low. I was completely impressed by the efficiency and professionalism of the hospital staff and I was fully informed of what the subsequent tests were showing. Randall was put on an external ventilator (which forced oxygen into his lungs via a tight mask rather than intubation but which was still very unpleasant) to keep his tissues sufficiently oxygenated.
Chest x-rays showed that his lungs were in remarkably good shape considering the long period that Randall had spent under general anesthesia but a CT-scan revealed that he had bilateral pulmonary embolisms. This means that he had small blood-clots in both lungs which was reducing the oxygenation of his blood and tissue. It was not clear, nor important, whether the embolisms had resulted from sitting still during the long-flights from New Zealand or from the surgery, but the clots may have been dislodged from his legs when he was walking.
Pulmonary embolisms are usually treated by some drugs that thin the blood and others that destroy the clots. The latter cannot be used after by-pass surgery but blood-thinning drugs would prevent the formation of any new clots and within a few weeks, his body would completely reabsorb the embolisms. Such therapy has to be applied carefully to ensure that his surgical wounds do not bleed but the doctors were confident that these drugs would improve Randall's condition.
He was initially given injections of heparin but he will be switched to an oral medication before leaving the hospital. While Cuomodin (warfarin) has been used for many years, it requires extensive blood-testing to establish suitable levels so Randall is lucky to be prescribed a newer, oral drug, Eliquis, which should be much simpler to use. Although, the embolisms may disappear relatively quickly, it remains to be seen whether Randall has to stay on the blood-thinners, or daily aspirin, for longer (or forever).
Similarly, it takes 4 to 6 weeks for his wired-together sternum to heal but how soon after that he can lift or strain his chest muscles will have to be evaluated after he sees the surgeon one month post-surgery. So our plans for visiting our daughters and returning to Tregoning are definitely on-hold. However, we could not have been in a better place for this to occur. Not only does Gainesville have excellent health-care facilities but we have many good friends here, who are generously offering to feed and house us for an extended period of time. Tregoning is in a good marina and we do not have to rush to move her to any other location.
We are not quite sure when Randall will be discharged from the hospital. His embolisms on Sunday quite set his recovery back so that he was as tired on Monday as he had been the first day after surgery and he was kept in bed-rest. Today (Tuesday) he has been sitting up in his chair but his walking is still very limited so I doubt that he will be leaving before Thursday. Randall is not ready to have visitors yet (talking is very tiring) but we are both greatly appreciative of all of the good-wishes that we have received.
The past week has been quite surreal but you will not hear us complain about bad luck. Considering all of the places we could have been when Randall's widowmaker was revealed, and the possible alternative consequences of its effect, we are astoundingly fortunate and heartily grateful to find ourselves sitting in a hospital in Gainesville, Florida.
So Thursday morning found us in a prep-room at the North Florida Regional Medical Center with Randall being readied for a heart-catheterization to inspect the state of the arteries providing blood to his heart. This was accomplished by a catheter inserted through his wrist and if there was any indication of arterial narrowing, a stent could be inserted immediately to open-up the vessel.
While Randall was wheeled upstairs for this procedure, I scurried across the street to have a routine mammogram (all good). On my return, I was a bit surprised to find Randall back in the prep-room receiving a chest x-ray and the staff looking rather less cheerful than when I had left. Imagine my surprise when the doctor showed me the images on his cell-phone that displayed two constrictions in Randall's left anterior descending artery, a vessel that feeds the left side of the heart, one of these being a 99% blockage. This artery supplies blood to such a large volume of heart-muscle that an obstruction in it is, rather disconcertingly, called a widowmaker because a complete blockage can result in a massive heart-attack and sudden death.
Of course, if I was surprised, Randall must have been completely shocked by the sudden flurry of tests that were being applied to him. He was not going to be allowed to leave the hospital but within a few hours he was wheeled upstairs to a room in the Cardiac-Vascular Unit which was going to be his home for the next few days. Open-heart, triple by-pass surgery was scheduled for the next morning so he had to undergo his third morning in a row of fasting.
Wow...what an unexpected change of plans this was turning out to be.
Randall's operation started just after noon on Friday and lasted for four hours. While I was in the Cardiac waiting-room, I was joined by my good friend Marilyn, who had been visiting her mother-in-law, Joan, who was recovering from double-pneumonia on the floor below. The surgeon reported that Randall's procedure had gone well very well and I was allowed to see him soon after he was returned to his room, while he was still on the ventilator and surrounded by pumps and monitors. Later in the evening, I saw Randall again when he was already off the ventilator and was able to recognize me and mouth “Hello” despite the heavy dose of pain-killers. I was able to return to Karen's knowing that Randall was in excellent hands and doing well.
Early on Saturday, I found that Randall was already sitting in a chair, which is an important part of the progression after heart-surgery, along with the regular use of inhalation- and exhalation-therapy devices (one of which sounds like a rather congested duck). He was pretty sleepy all day so I was able to catch-up with various friends between visits.
Arriving early on Sunday, I was a bit surprised to find him using an oxygen mask. Apparently, he had felt a bit dizzy when he been encouraged to walk at 4:30 am. Walking is a critical part of the post-heart-surgery therapy so it is attempted several times each day and is carefully monitored. When it was time for his walk at noon, I accompanied him and his nurse down the hallway and he seemed to be doing really well but as we started returning to his room, he declared that he had gone too far and started to crumple. Sally and I caught him and lowered him to the floor so that he did not hurt himself but I was pretty frightened when one of the many nurses that suddenly appeared from the neighboring Critical-Care Unit asked whether he had suffered a stroke.
Thankfully Randall quickly regained consciousness and was immediately able to squeeze his hands and move his feet as directed. His pulse and blood-pressure were at acceptable levels but for some reason, the concentrations of oxygen in his tissues had dropped too low. I was completely impressed by the efficiency and professionalism of the hospital staff and I was fully informed of what the subsequent tests were showing. Randall was put on an external ventilator (which forced oxygen into his lungs via a tight mask rather than intubation but which was still very unpleasant) to keep his tissues sufficiently oxygenated.
Chest x-rays showed that his lungs were in remarkably good shape considering the long period that Randall had spent under general anesthesia but a CT-scan revealed that he had bilateral pulmonary embolisms. This means that he had small blood-clots in both lungs which was reducing the oxygenation of his blood and tissue. It was not clear, nor important, whether the embolisms had resulted from sitting still during the long-flights from New Zealand or from the surgery, but the clots may have been dislodged from his legs when he was walking.
Pulmonary embolisms are usually treated by some drugs that thin the blood and others that destroy the clots. The latter cannot be used after by-pass surgery but blood-thinning drugs would prevent the formation of any new clots and within a few weeks, his body would completely reabsorb the embolisms. Such therapy has to be applied carefully to ensure that his surgical wounds do not bleed but the doctors were confident that these drugs would improve Randall's condition.
He was initially given injections of heparin but he will be switched to an oral medication before leaving the hospital. While Cuomodin (warfarin) has been used for many years, it requires extensive blood-testing to establish suitable levels so Randall is lucky to be prescribed a newer, oral drug, Eliquis, which should be much simpler to use. Although, the embolisms may disappear relatively quickly, it remains to be seen whether Randall has to stay on the blood-thinners, or daily aspirin, for longer (or forever).
Similarly, it takes 4 to 6 weeks for his wired-together sternum to heal but how soon after that he can lift or strain his chest muscles will have to be evaluated after he sees the surgeon one month post-surgery. So our plans for visiting our daughters and returning to Tregoning are definitely on-hold. However, we could not have been in a better place for this to occur. Not only does Gainesville have excellent health-care facilities but we have many good friends here, who are generously offering to feed and house us for an extended period of time. Tregoning is in a good marina and we do not have to rush to move her to any other location.
We are not quite sure when Randall will be discharged from the hospital. His embolisms on Sunday quite set his recovery back so that he was as tired on Monday as he had been the first day after surgery and he was kept in bed-rest. Today (Tuesday) he has been sitting up in his chair but his walking is still very limited so I doubt that he will be leaving before Thursday. Randall is not ready to have visitors yet (talking is very tiring) but we are both greatly appreciative of all of the good-wishes that we have received.
The past week has been quite surreal but you will not hear us complain about bad luck. Considering all of the places we could have been when Randall's widowmaker was revealed, and the possible alternative consequences of its effect, we are astoundingly fortunate and heartily grateful to find ourselves sitting in a hospital in Gainesville, Florida.
Comments
| Vessel Name: | Tregoning |
| Vessel Make/Model: | Morgan Classic 41 |
| Hailing Port: | Gainesville, FL |
| Crew: | Alison and Randall |
| About: | We cast-off from Fernandina Beach in north Florida on 1st June 2008 and we have been cruising on Tregoning ever since. Before buying Tregoning, both of us had been sailing on smaller boats for many years and had worked around boats and water throughout our careers. |
| Extra: | “Tregoning” (rhymes with “belonging”) and is a Cornish word (meaning “homestead of Cohnan” or “farm by the ash trees”) and was Alison's mother’s middle name. Cornwall is in southwest England and is where Alison grew-up. |
Tregoning's Photos - Main
 |
Extra photographs from our three-week campervan tour of the South Island from November 15th to December 5th 2015
217 Photos
Created 4 January 2016
|
 |
Random pictures from our month spent on the islands of Hiva Oa, Tahuata, Ua Pou, and Nuku Hiva
45 Photos
Created 18 July 2015
|
 |
Random pictures from our month spent in 4 Tuamotu Atolls; Ahe, Fakarava, Tahanea, and Toau
32 Photos
Created 1 July 2015
|
 |
Some of the birds, fish, reptiles, and mammals (and others) that we have seen in Mexico
74 Photos
Created 5 May 2014
|
Tregoning

Who: Alison and Randall
Port: Gainesville, FL